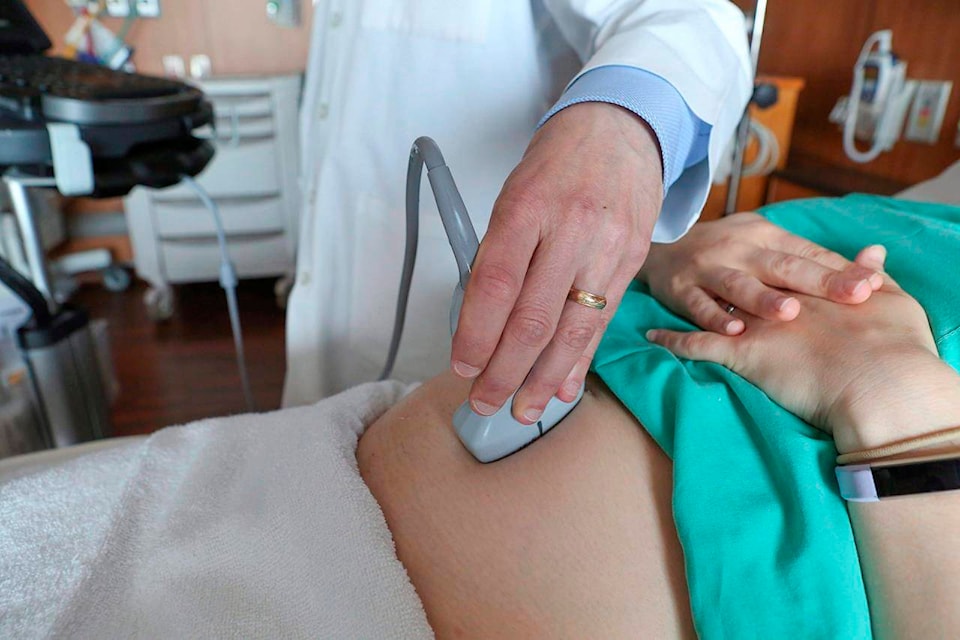
Sexual health experts across Canada are concerned the COVID-19 pandemic may be causing women to neglect their reproductive care.
A global crisis isn’t the time to postpone essential appointments, they say.
“The message should be loud and clear that critical screening practices absolutely should continue,” said Dr. Lori Brotto, a psychotherapist and the director of the UBC Sexual Health Laboratory in Vancouver.
“Women are on a fixed schedule for a reason and that regular surveillance is very critical.”
Pap smears that screen for cervical cancer and mammograms, which can detect breast cancer, are particularly important for women who either have a family history or have had irregular tests in the past.
Reasons for wanting to delay appointments during the pandemic can vary, Brotto said. Some may resist out of fear of visiting a medical facility while others are facing financial burdens that make accessing care and treatment more difficult.
No longer having a job or health benefits to cover prescription medication like birth control can be particularly problematic.
Dr. Rachel Spitzer, an obstetrician/gynecologist at the University of Toronto and Mount Sinai Hospital, says it’s those financial obstacles that are more concerning now.
“Truthfully, I’m not worried about somebody waiting three and a half years to get their pap instead of three years,” Spitzer said. “But I am very worried about people running out of contraception and maybe not being in a relationship where they can have the autonomy to avoid intercourse and having an unplanned pregnancy.”
Spitzer said pregnancy care and abortion services have been “prioritized quite well” in Canada, but the pandemic can affect access to reproductive health in other ways.
Not having a safe means of transportation is one, and teenagers, Spitzer said, can be especially affected if they’re stuck at home and unable to access care privately.
“I think contraception is a big concern … and I do worry about access for people who have lost their jobs — what happens if suddenly you can’t afford your contraceptive anymore?” Spitzer said.
“All of those intricacies become highly complex at a time like this, where getting places is more difficult or leaving the place that you’re at is more difficult. And so we worry significantly about people experiencing intimate partner violence also.”
Rachel Skolnik, an OB/GYN resident with the University of Toronto, says police-reported domestic violence instances have been on the rise since the start of the coronavirus pandemic.
A United Nations Population Fund projection released last week said 31 million additional cases of gender-based violence worldwide “can be expected if the lockdown continues for at least six months.”
“So now more than ever, we need to be screening patients for intimate partner violence,” Skolnik said.
Skolnik is one of many University of Toronto OB/GYN residents collaborating with the student-led COVID-19 Women’s Initiative (CWI) that advocates for gender equity.
READ MORE: Trudeau announces $240M funding for online mental health platform, virtual healthcare
Skolnik and her colleagues created a map on the CWI website that highlights which clinics are open throughout the Greater Toronto Area, and which services are being provided, including contraception and IUD insertion, abortions and STI screening.
“There’s a lot of uncertainty around the availability of services and what constitutes an essential medical service,” Skolnik said. “We felt that one of the (problems) is actually just knowing where to go and what is available, and that’s evermore an issue during a pandemic.”
Many of those Toronto sexual health clinics — and others across the country — have moved some of their services to a virtual platform.
Initial consultations and prescription refills can be done online via video appointment, unless there are extraneous circumstances, and if a patient does require in-clinic care, safety precautions are being taken on and off-site, including a COVID-19 screening over the phone.
Some clinics will also urge patients to wear masks and appointments are scheduled to ensure waiting rooms are essentially kept empty.
“Patients are spending less time in the clinic, encountering less people in waiting rooms, and they’re out of the clinic fairly quickly,” Spitzer said.
Patients are also asked to come in alone, meaning they won’t have the support of a friend or family member with them, even during some anxiety-provoking appointments.
READ MORE: B.C. unveils $5M for mental health supports during the COVID-19 pandemic
While Spitzer said this can be tough for people to deal with, she encourages her patients to video call a supportive friend during the appointment. Translation services, which would usually happen face-to-face, can also be arranged over the phone.
Brotto, also a sex therapist who continues to see clients remotely, said there can be downsides to limiting face-to-face interactions with doctors.
“People use that opportunity to talk about things like violence in their relationships or other issues about their sexual health,” she said. “So it remains to be seen what the impact is going to be — is this going to result in people holding back and not getting the care they normally would?
“Or is moving online actually going to increase (access) because now people who live in more remote areas are able to get care?”
Spitzer said it’s important for people to know that urgent sexual health services are still available to them. And anyone unsure how to proceed with an urgent request should call a clinic or their doctor to ask.
“Let us be the ones to help determine the urgency,” she said.
“We’re certainly not closed for business and nobody should be neglectful of their health, especially when it comes to their reproductive health.”
Melissa Couto, The Canadian Press