MIKE YOUDS
SPECIAL TO THE NEWS
Port Alberni, considered a leader among B.C. communities in its opioid crisis response, has to expand services and work toward greater public engagement to move beyond “just saving lives,” a public forum heard Thursday night.
The presentation at the Barclay Hotel began on a tragic note. Tseshaht Chief Counsellor Cynthia Dick said two band members, one from Tseshaht, the other from Hupacasath, overdosed earlier in the week.
“The Hupacasath did not make it,” she said.
First in a series of gatherings held by CAT — the Community Action Team responsible for developing a multi-faceted response to the crisis — the 90-minute panel discussion centred on stigmatization. Social attitudes that alienate, marginalize and vilify are considered a major obstacle to harm reduction and recovery from substance addiction.
READ: Alberni group focuses on stigmatization as biggest barrier to opioid crisis
READ: Province announces $1.5 million in funding to combat overdose epidemic
Those views are understandable, said Dr. Paul Hasselback, medical health officer.
“We kind of respect that people are in different places,” he told an audience of about 50.
Within a few short years, communities have had to come to grips with the problem in all its tragedy, controversy and complexity, he said.
“And everybody in a community comes through it at a different pace,” he said. “Some are very prepared to embrace it from the beginning, others as they become more aware of what’s occurring, others are grappling with the consequences of what they see around because this has become so real and so visual and physical within the community.”
The crisis has brought a profound sense of loss in many ways. “Not just a loss of friends and family. We have lost 50 individuals — five zero —in this community in the last 10 years, most of that just in the last couple of years,” he said.
Loss is also felt through “impacts on businesses, the view of the street, the divisiveness that occurs, the acrimony and conflict that occurs within a community. Hence the importance of coming together like this and having open, free dialogue.”
Hasselback pointed to the possibility of a “therapeutic community,” an example set by Portugal, as the proper and humane course.
“Everybody is involved in caring for each other,” Hasselback said. “There is the challenge for Port Alberni. How can you, not just as a community but as an individual, embrace the needs of everyone in this community and be part of their therapeutic journey irrespective of where they are on that substance use pathway? We’ve seen huge changes in the last few years. We’ve got a long way to go.”
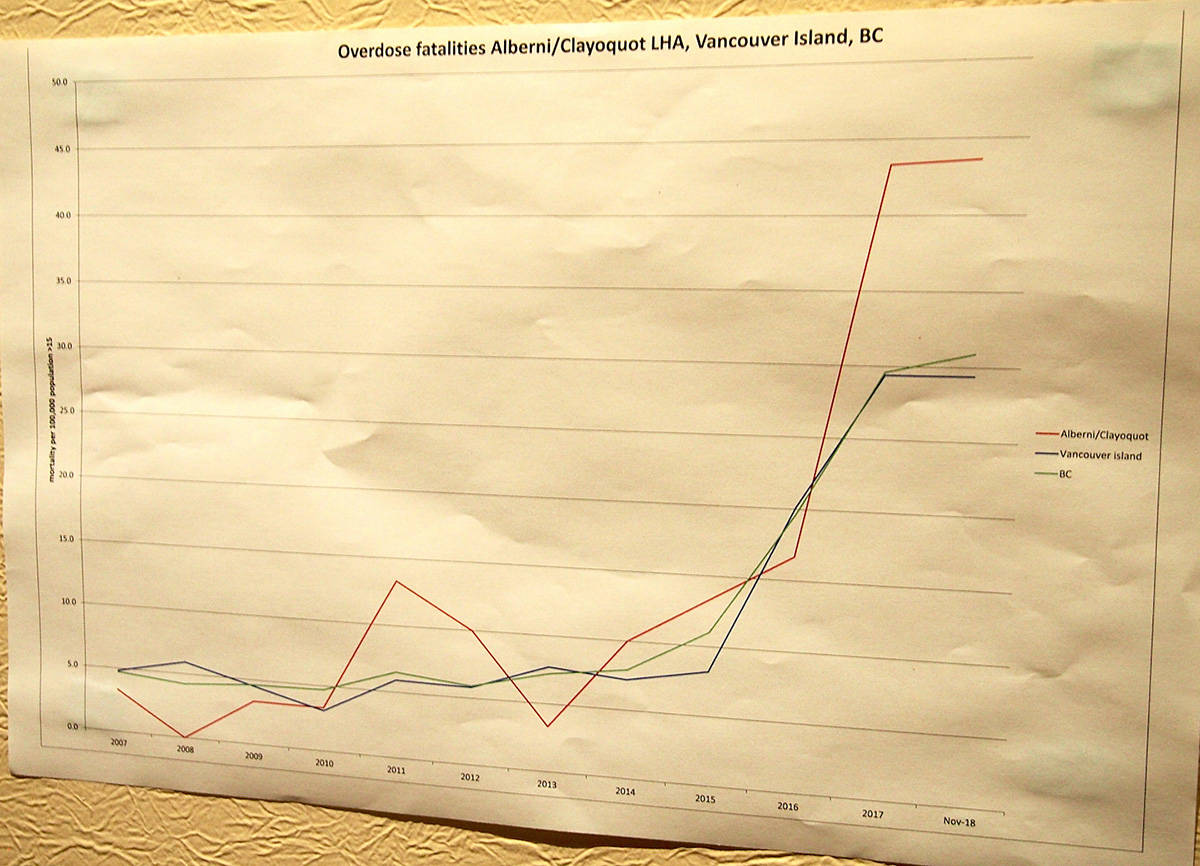
The city’s overdose rate is about 50 percent higher than the rest of B.C., an unacceptable rate, he said. Overdoses are 10 times what they were five years ago. About 500 people in the region have opiate use disorder. Roughly 200 may be on treatment. About 300 are injecting several times a day.
The vast majority of overdoses, which are common, occur in private residences. Those dependent on opiate use don’t inject to get high but to avoid sickness when they come down, the MHO said.
Speaking on behalf of MP Gord Johns, Sarah Thomas said the federal government needs to step up its response to the crisis by decriminalizing personal possession, providing safe access and mobilizing the sort of resources levelled against SARS, H1N1 and AIDS. Johns is petitioning the House to act accordingly.
Debra Hamilton, CAT co-chair, wondered why Ottawa hasn’t declared a public health emergency similar to the one in place in B.C. for the last three years.
“What are they waiting for?”